Fighting the opioid crisis has been saved

Fighting the opioid crisis An ecosystem approach to a wicked problem
15 August 2016
Health and criminal justice organizations aren’t the only ones who should involve themselves in solutions for opioid abuse. Here’s how they can join forces with innovators, technologists, and experts beyond traditional stakeholder groups to help fight the US opioid crisis.
Introduction

Most people know of the game called Six Degrees of Kevin Bacon. Based on the concept of "six degrees of separation," it was invented by three college students who believed that every person in the entertainment industry stands no more than six acquaintance links away from the actor Kevin Bacon.1 Now, consider a similar exercise focused on the much-publicized opioid and heroin epidemic. Many people today, the authors included, find themselves just “one degree” away from this calamity, having seen friends, family members, and communities devastated by opioid abuse and heroin use.
Learn More
Listen to the related podcast
A crisis that has spread so broadly, and penetrated so deeply, demands wide-scale, integrated solutions, with contributions from all impacted sectors. The concept of an “ecosystem” provides a metaphor for the kind of collaboration needed to take on the opioid epidemic. Having studied several other solution ecosystems that have made the most progress in addressing societal problems, Deloitte finds that they often have five elements in common.2 They:
- Engage a broad community of “wavemakers” to innovate, convene, and fund its own solutions.
- Establish an ecosystem integrator to “hold the whole” and create the space for aligned action by others.
- Attack the problem with a portfolio of interventions.
- Create an innovation engine to drive ideas for solutions that upend the problem.
- Develop solutions embedded in well-functioning markets.
Government agencies, communities, and health care organizations engaged in the fight to end the opioid crisis may wish to consider incorporating these elements into their strategies.
The scale of the opioid crisis
A few gut-wrenching facts illustrate how this crisis touches the average American:
- In 2012, health care providers wrote 259 million painkiller prescriptions, enough to give every adult in the United States his or her own bottle of pills.3
- The United States has less than 5 percent of the world’s population, yet consumes roughly 80 percent of the global opioid supply.4
- The number of prescriptions for opioids has increased from 76 million in 1991 to nearly 207 million in 2013.5
- Drug overdose deaths reached record highs in 2014, fueled in large part by the abuse of narcotic painkillers and heroin.6
- In 2014, 47,055 Americans died from drug overdoses, an increase of more than 14 percent from 2013. Of those deaths, 28,647—or 61 percent—involved the use of opioids. From 2000 to 2014 nearly half a million people died from overdoses in the United States.7
- In 2014, there were approximately one-and-a-half times more drug overdose deaths than deaths from motor vehicle crashes.8
Anecdotal examples also abound. One cannot miss the many news stories, articles, documentaries, political speeches, and state legislative efforts devoted to opioid and heroin addiction, or the untimely deaths of individuals linked to opioids. The opioid and heroin epidemic touches nearly every American. Some are prescribed opioids for pain relief, some are battling opioid and heroin dependency and addiction, while others have lost a loved one or friend to an overdose. It’s hard to believe that just two decades ago, when opioids were mainly prescribed as end-of-life cancer drugs, most Americans felt little connection to the problem of opioid use and heroin abuse.
The opioid epidemic cuts across every sector of society. Much like an environmental disaster—the ongoing release of toxic chemicals into air and water, for example—it endangers not just one population, but an entire social ecosystem, a community of interconnected individuals and interests. Such a broad crisis requires an equally broad response, with collaboration from stakeholders in all of the ecosystem’s many sectors.
The impact of the epidemic
For too long we’ve viewed drug addiction through the lens of criminal justice. The most important thing to do is reduce demand. And the only way to do that is to provide treatment—to see it as a public health problem and not a criminal problem.—President Barack Obama, speaking at the National
Prescription Drug Abuse and Heroin Summit,
March 2016
President Obama’s statement highlights the critical shift underway across the country, as communities start to treat addiction as a public health crisis. The impacts of the epidemic extend far beyond the domains of substance abuse treatment and criminal justice. Opioid addiction eats at the core of our communities—it strains our health care resources, stresses our child welfare systems, reduces the economic vitality of American families, and drains our first responders. It requires governments to continually shift resources to respond to emergent issues.
The opioid and heroin epidemic touches a plethora of government programs, impacting children and families, law enforcement professionals, educators, health care providers—not to mention taxpayers. (For details, see the sidebar “The widespread impact of opioid abuse and heroin use.”)
Table 1. The widespread impact of opioid abuse and heroin use
Medicaid |
|
Child welfare |
|
Workforce and economic development |
|
Criminal justice |
|
Treatment centers |
|
Workers’ compensation |
|
Adolescents and education |
|
Public health |
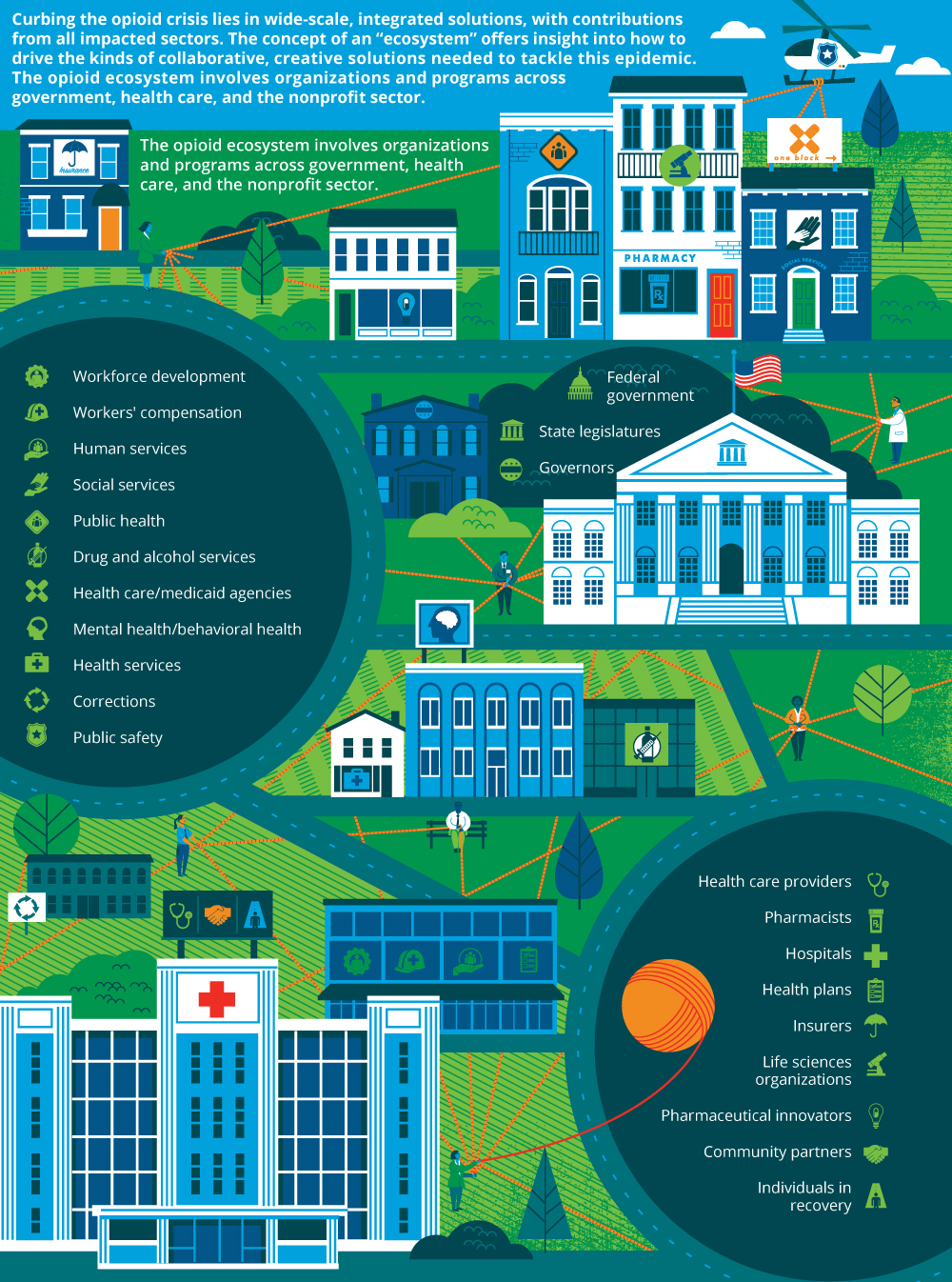
To address these far-reaching impacts, state and federal agencies have devoted a staggering volume of resources to fighting the opioid and heroin epidemic. Figure 1 depicts some of the organizations and programs involved in targeting the opioid crisis.
Figure 1. The opioid crisis ecosystem
States across the country have undertaken a number of measures to combat the epidemic. They include:
- Prevention efforts: Ranging from mandatory prescription drug monitoring programs (PDMP) to prescriber guidelines
- Treatment efforts: Including expanded access to treatment and easier access to the overdose antidote naloxone
- Legal and criminal justice efforts: By, among other initiatives, offering early release to individuals in prison who are addicted to opioids, so they can obtain managed treatment, and prosecuting individuals who prescribe opioids illegally
Despite the vast breadth and depth of these efforts, the United States has not turned the tide on the epidemic.
A wicked problem?
Given the widespread impact of the problem, curbing the opioid crisis lies in wide-scale, integrated solutions, with contributions from all impacted sectors. The concept of an “ecosystem” offers insight into how to drive the kinds of collaborative, creative solutions needed to tackle this epidemic.
The term “ecosystem,” as first used in the field of botany, refers to a localized community of living organisms that interact with one another and with their particular environment of air, water, mineral soil, and other elements. These organisms influence one another and their terrain; they compete and collaborate, share, and create resources and co-evolve. When faced with external disruptions, they adapt together.24
The concept of an “ecosystem” offers insight into how to drive the kinds of collaborative, creative solutions needed to tackle this epidemic.
Business strategist James Moore noticed the parallels to the world of commerce in the 1990s. In a 1993 article in the Harvard Business Review, he wrote, “I suggest a company be viewed not as a member of single industry but as a part of a business ecosystem that crosses a variety of industries. In a business ecosystem, companies co-evolve capabilities around a new innovation: They work cooperatively and competitively to support new products, satisfy customer needs, and eventually incorporate the next round of innovations.”25
Nonprofits and governments have embraced the ecosystem concept as a way to address what are often called “wicked problems.” Wicked problems are generally identified through a combination of unique characteristics;26 we have highlighted some of those characteristics that are most relevant to the opioid crisis:27
- Different parties have different definitions of the problem: Demand or supply issue? Prevention or treatment focus? Criminal justice or health orientation? While most all involved can agree on some basic outcome measures in the fight against the opioid crisis—such as a reduction in overdoses—there is no agreement across the ecosystem on the root of the problem. When you couple that with a diverse set of actors you get differing definitions of the problem and hence differing definitions for what “success” really means.
- The sources are diverse. The source of the opioid epidemic is not just due to the inflow of illegal drugs and the creation of new prescription drugs. The complex reality is that the crisis is driven by many problems, such as lack of alternative pain management treatments for sufferers of chronic pain, loose prescribing practices, inadequate training for physicians and consumers, and treatment programs and reimbursement strategies that haven’t evolved to support the longer-term treatment needed for addiction to opioids.
- The problem is emergent and shifting. With growth in the use of opioids over the last 20 years, the nature of the crisis has changed. Opioid addiction no longer springs mainly from recreational use of illicit drugs; many people now become addicted while using legally prescribed painkillers. As opioid use increased, and users became desperate for supply sources, some physicians began to set up “pill mills”—storefront offices established with the sole purpose of churning out prescriptions for opioids. Then law enforcement cracked down on the abuse, and many doctors came under more scrutiny for prescribing practices, making the drugs more difficult to obtain. Individuals struggling with addiction turned from prescription pills to the street drug, creating a fresh opportunity for heroin distributors. Once focused primarily on urban areas, their networks quickly adapted to the new demand, targeting communities suffering from economic loss and hardship, including rural and rust belt communities.28And today, governments face a new challenge—how to follow up with patients after the use of the overdose antidote naloxone, in order to help curb their addiction long term. The opioid crisis is a criminal justice crisis, a physical health crisis, a behavioral health crisis, a public health crisis, and a human services crisis. Each piece of it requires a separate set of strategies.
- There will never be one answer. An emergent and shifting problem by definition means that solutions have to be flexible, creative, and continually refreshed, with engagement from all parties in the ecosystem. Part of the reason there will never be “one answer” to address the opioid crisis is because of the varied demographic factors that contribute to the challenge. Research shows that many different social determinants, including interpersonal, household, and community dynamics, strongly influence substance abuse.29 For example, heroin kills more people in New England and the Midwest than in the rest of the country, and heroin victims are more likely to be men in their 20s and early 30s. Prescription opioids, on the other hand, impact people across the country, especially people aged 45–54 and including a substantial number of women.30 Effective prevention strategies differ between rural and urban communities, and whether the addiction begins with abuse of prescription drugs or heroin.31
Recent efforts, driven by key governors across the country, have recognized the need for multifaceted strategies that consider geographic differences. For example, Pennsylvania’s strategies extend from health to corrections to education to emergency management. In Massachusetts, the 2014 task force identified more 35 recommendations involving data, policy action, prevention, intervention, treatment, and recovery. Many other states have developed similar plans involving the entire state government.
What can we learn if we view the opioid crisis as an ecosystem?
Researchers have found five common elements in effective ecosystem interventions. The five elements, and their implications for addressing the opioid epidemic, are described below.32
1. Engage a broad community of “wavemakers” to innovate, convene, and fund its own solutions
Across the country, stakeholders in the opioid crisis are coming together through commissions, roundtables, and conferences. They analyze the root causes of the problem, highlight successful solutions, and make recommendations for state, local, and federal government agencies. As these convening groups develop and shift into implementation, it is critical that they engage new partners and collaborate on novel solutions that stakeholders can implement themselves. Partners at the table for discussions of opioid abuse should not be limited to health and criminal justice stakeholders; new and unusual partners should be brought into the fold, including people who are in recovery. Which groups are uniquely impacted by the crisis? Who are some of the common stakeholders across all sectors? How might one engage innovators, technologists, and experts drawn from beyond the traditional stakeholder groups?
One way to achieve a healthy ecosystem is to make sure that the success of each party depends on the success of all other parties.
One effective model comes from the world of children’s behavioral health, which has adopted a “systems of care” philosophy. This approach recognizes that it takes collaboration by a wide range of partners to appropriately serve the shifting and complex needs of children. Recent reports show that the “systems of care” approach has realized a positive return on investment, in terms of both cost avoidance and improved outcomes.33
Stakeholders should try to implement solutions that benefit everyone at the table. Solutions that are “single-threaded” through government agencies will likely have limited impact. One way to achieve a healthy ecosystem is to make sure that the success of each party depends on the success of all other parties. For example, workers’ compensation programs are often viewed as benefits programs, providing income replacement for injured workers until they can return to work. However, given the volume of opioids they saw being prescribed for work-related injuries, workers’ compensation insurers were some of the first organizations to recognize the critical role that physicians played in preventing opioid addiction.
Today, workers’ compensation insurers are beginning to utilize advanced detection tools. Thanks to their unique position in the ecosystem—where they touch health care, consumers, and governments—they are effectively leveraging state and federal guidelines, physician education, and advanced analytics to help prevent dependency and addiction.
2. Establish an ecosystem integrator to “hold the whole” and create the space for aligned action by others
State governors and their administrations are increasingly serving as “integrators” in the anti-opioid ecosystem. State commissions, such as the Commonwealth of Virginia Governor’s Task Force on Prescription Drug and Heroin Abuse, the Commonwealth of Massachusetts Governor’s Opioid Working Group, and New York’s Heroin and Opioid Task Force, are helping to drive real action. They achieve this through improved coordination and alignment of strategies focused on opioid abuse and heroin use prevention, intervention, treatment, recovery, and enforcement. Given the attention these commissions have received, and the resources their work has attracted, state leaders might wish to consider how such bodies can drive ongoing implementation and innovation after they deliver their final reports. Through working sessions, implementation groups, and coordinated action plans at the governor’s level, government can integrate the activities of executive agencies, community organizations, and health care providers, making the overall effort more effective.
The integrator role, however, need not be limited to governments. Give the wide-scale impact of the opioid crisis, other organizations may be able to step into the role of integrator. Foundations or companies that focus on public health, economic development, or the welfare of children and families may be well-positioned to drive collaboration across the ecosystem. They may also be particularly adept at tailoring efforts to the unique needs of a community or region.
3. Attack the problem with a portfolio of interventions
Successful ecosystems recognize that working together doesn’t necessarily mean agreeing on one best solution. Instead, it means coordinating a full portfolio of strategic interventions which, when taken together, have the best chance of hitting the goal. For example, in recent years, anti-opioid initiatives have enhanced their focus on education. They have done so with the understanding that it isn’t enough just to educate primary care physicians: Effective physician and patient education on the adverse impacts of opioids involves multiple players and strategies.
In 2012, Physicians for the Responsible Prescribing of Opioids (PROP) submitted a petition to the Food and Drug Administration (FDA) requesting labeling changes for all opioids prescribed for non-cancer pain. In 2013, the Drug Enforcement Agency (DEA) and the National Association of Attorneys Generals endorsed this proposal, asking the FDA to place a “black box warning” label on opioids prescribed to pregnant women. In March 2016, the Centers for Disease Control and Prevention (CDC) issued new guidelines for prescribing opioids for chronic pain. In addition, state agencies, federal agencies, physicians, and medical colleges have been updating their educational materials to better warn physicians about the risks of opioid abuse and addiction. This portfolio of interventions has prompted pain clinics and emergency rooms to stop, or drastically reduce, the use of opioids for chronic conditions. Following a multipronged educational effort, one health plan reported a 29 percent decline in high-risk members prescribed opioids.34
Governments and health providers are developing protocols that acknowledge the need to take a “portfolio of interventions” approach when trying to cure addiction. Detoxification rarely solves the problem on its own, as individuals who go through detox programs often relapse later. A more effective strategy combines a number of interventions—which may include detoxification, abstinence-oriented treatment, and/or supervised opioid replacement treatment, such as methadone. Although this proposal has sparked controversy, in October 2015 Massachusetts Governor Charlie Baker introduced legislation giving hospitals more flexible power to hold an individual against his or her will for three days after the administration of an overdose antidote. One of the most interesting aspects of this policy is that it emphasizes the shift in focus from a criminal justice perspective to a health care one, as it brings clinicians directly into the decision-making process for this type of treatment.35
Whether the solutions involve education, treatment, or enforcement, efforts to address any aspect of the opioid epidemic are likely to be most successful when they employ a portfolio of interventions, rather than a single, “silver bullet” solution. For example, research shows that for some people, combining medication-oriented treatment with behavioral treatments is the most effective way to address addiction.36 That makes it critical to engage multiple partners across the ecosystem.
4. Create an innovation engine to drive ideas for solutions that upend the problem
Groups fighting the opioid epidemic try to approach the problem from every possible angle. But members are the first to admit that without new solutions, the epidemic probably won’t let up anytime soon.
New solutions emerge when partners in an ecosystem interact cooperatively and competitively to drive innovation. Governments should consider going beyond roundtables and commissions: They need to create opportunities for new partnerships to form. Examples of successful innovation engines that have been used to address other social problems include:
Prize-based challenges: Incentives for innovations that produce public value have seen significant success. Organizers define the challenge, offer a prize, and then open the competition for individuals or teams to offer solutions. This model has worked so well in addressing problems that range from nursing home care to space travel that the US government has established its own platform for hosting challenges—Challenge.gov. Turning an aspect of the opioid epidemic into a challenge could help drive the sorts of cooperation and competition this complex issue requires. In fact, the Substance Abuse and Mental Health Services Administration (SAMHSA) has already seen strong participation in two recent challenges launched around recovery support and prevention.37 A local organization might challenge the community to find a way to provide more widespread access to naloxone, or a biotech organization might offer a prize for solutions that encourage Americans to dispose appropriately of their leftover opioid prescriptions (which sit, at risk for misuse, in 60 percent of medicine cabinets across the country).38
Pay for Success (PFS): This is an approach for social services that ties payment for services to outcomes. Governments are increasingly partnering with funders to explore this model of delivery. In its simplest form, it means that instead of paying an organization for each service rendered or via a grant, the government pays a service organization—wholly or in part—based on performance against particular metrics. Since many social service organizations lack the base funding to support their efforts, this model calls upon foundations or corporations to provide startup loans or outright grants, bridging the gap until the service organization earns its performance-based payments. Pay for Success projects are being implemented to address issues such as homelessness, recidivism, and early childhood education.39 The model is helping to forge new partnerships: A review of current projects shows active engagement from corporations, foundations, and social services agencies.
Given its progress so far in tackling intractable issues such as homelessness, this model may have something to offer the fight against the opioid epidemic. Imagine a Pay for Success model to reduce relapses for those in recovery. Such an effort could bring together employers, government, health care providers, and social services agencies—all of whom have an interest in helping individuals recover fully.
Advanced analytics: Governments today are collecting more and more information related to opioid addiction. From databases that monitor prescription drugs and Medicaid enterprise solutions, to systems that track licensing violations and digital archives of vital records—all these data sets contain critical information about opioid use and abuse. Data scientists are connecting data from these different sources and then using it in new and innovative ways to help identify patients’ pill-seeking behaviors, and prevent opioid addiction and dependency before the habits form. These approaches may offer ways to engage stakeholders across traditional boundaries, leading to new solutions.
For example, prescription drug monitoring programs contain databases of prescription information, which can be updated and accessed by providers and pharmacists. They offer an avenue for data-driven decision making and accountability in an ecosystem context. Effective prescription drug monitoring programs can keep a broad spectrum of stakeholders informed and create a common body of truth. In one recent study of prescription drug monitoring programs, implementation of this technology correlated with a 30 percent drop in opioid prescriptions.40
At the same time, government leaders should keep in mind that new solutions may bring unintended consequences. For example, as mentioned previously, a number of states have worked aggressively to close illegal “pill mills.” Although this drastically reduced the illicit supply of opioids, it also left large numbers of individuals suffering from addiction without detoxification options. Unfortunately, some of those sufferers turned to heroin to feed their addictions. Thus, a win on the opioid abuse front became a loss on the heroin trafficking front. When a community considers any intervention, it must evaluate the plan and then monitor its implementation from the perspective of the entire ecosystem.
5. Develop solutions embedded in well-functioning markets
In efforts to address other “wicked problems,” suc-cess has relied not just on effective interventions, but on interventions that were sustainable in the context of real-world markets. For example, the battle against malaria depends on having viable markets for the purchase and sale of mosquito nets, medical treatments, and diagnostic devices. Similarly, solutions to the problems of adequate housing in slums, sanitation in poor communities, and traffic congestion have emerged when the solution could be brought to bear “organically, sustainably, and profitably.”41 Clearly, there is signi-ficant room for innovation in the fight against opioid abuse and heroin use. Whether one is trying to reduce cost of long-term treatment, or figure out how to improve access to the overdose antidote naloxone, the challenges offer opportunities for market-oriented solutions.
One such opportunity may already be taking shape. The US health care market is transitioning—albeit slowly—to “value-based care,” a model that links provider payments to patient outcomes rather than volume of services. This model might also drive better outcomes for people suffering from addiction. Today, many programs set rigid rules about how long treatment lasts and where patients receive it. For instance, a program might limit in-patient care to 21 days and then provide minimal out-patient support. But opioid addiction requires more intensive care than this, over a longer period. Recent research indicates that individuals in recovery may suffer relapses two, three, or even four years after treatment. What if payment to a doctor or a treatment program were linked directly to patient outcomes? If the movement to a value-based health care model is successful, health care providers might find more effective and sustainable ways to treat patients recovering from opioid addiction.
Other new solutions that rely on products available in the marketplace are currently being tested in pockets across the United States. For example, Illinois recently passed legislation to launch a pilot program that will have participating pharmacies dispense medications that contain hydrocodone in bottles that are secured with combination locks.42 The cost of the locking devices and the additional effort that pharmacies must expend to use them will likely be key factors in the sustainability of the program. Other promising products already on the market include pouches that can be used to safely dispose of medication43 and long-acting treatments for opioid addiction. Solutions that rely on custom-built tools might work well in pilot implementations. But to make these solutions sustainable, the tools must be available for purchase, at prices that are viable in a functioning market. Ecosystems need to create a climate in which developers of innovative tools against opioid addiction can thrive in the open market.
Conclusion
The opioid epidemic is a “wicked problem” of the worst kind. It hurts all of us, every day, as it cuts lives short, rips families apart, and leaves loved ones in mourning. Even as the number of deaths continues to rise, physicians keep prescribing opioids to their patients, knowing that there are few alternative pain management treatments that are as quick to use.
An ecosystem approach could become the best hope in the battle against opioid addiction. From engaging new partners in the fight and aligning action across the ecosystem, to using a portfolio of interventions, driving innovation, and using markets to support sustainable solutions, the ecosystem is likely to generate the most powerful response. This collaborative approach inspires all stakeholders—across the boundaries of public health, criminal justice, economic development, and human services—to act as a single, integrated community and point the way toward powerful new solutions. We need those innovations to ensure that people in future generations all stand far more than six degrees apart from the opioid and heroin epidemic.
About the DELOITTE Center for Government Insights
The Deloitte Center for Government Insights shares inspiring stories of government innovation, looking at what’s behind the adoption of new technologies and management practices. We produce cutting-edge research that guides public officials without burying them in jargon and minutiae, crystalizing essential insights in an easy-to-absorb format. Through research, forums, and immersive workshops, our goal is to provide public officials, policy professionals, and members of the media with fresh insights that advance an understanding of what is possible in government transformation.